
Transcranial Magnetic Stimulation for depression, known simply as TMS Therapy, is a groundbreaking therapy that is a safe, effective, and pain-free method for treating depression, addiction and other mental health conditions. It also goes by the name, Repetitive Transcranial Magnetic Stimulation (rTMS).
Left untreated, poor mental health issues can be extremely debilitating. It can be even more frustrating when frontline treatment methods, such as antidepressant medication, fail to alleviate the associated symptoms.
Depression is among the most common mental health issues in the United States and the leading cause of disability in people between the ages of 15 and 44.
The symptoms of depression are often misunderstood. We know for certain it can cause a feeling of overwhelming sadness, hopelessness, and may leave a person experiencing severe exhaustion.
Depression is also known to create other health problems for people, especially when not properly treated.
It’s not uncommon for those living with depression to self-medicate their symptoms with drugs and alcohol, which can easily develop into a full-blown addiction, in addition to the already present mental health condition.
In fact, self-medicating with other substances usually amplifies the symptoms of depression and makes them even worse over time.
The presence of a mental health disorder and a substance use disorder is referred to as a co-occurring disorder, requiring a dual diagnosis treatment program for recovery to be successful.
Sometimes it’s unclear which condition developed first, but there’s overwhelming evidence that the symptoms of each disorder only serve to magnify and worsen the symptoms of the other.
Neither depression nor addiction needs to be a life sentence, however. There are effective treatment methods for both, and many people generally make a full recovery.
For the estimated one-third of patients living with treatment resistant depression, TMS therapy is an especially effective treatment option, according to a study published in Dialogues in Clinical Neuroscience.
How Does TMS Therapy Work?
Though TMS Therapy Transcranial Magnetic Stimulation may sound intimidating, the process is an outpatient procedure and completely noninvasive and pain free.
There is no anesthesia required and patients are awake and alert during the entire process. Even more important is the fact that there are very few side effects associated with TMS Therapy treatments.
TMS Therapy directs magnetic energy pulses, the same kind used in MRIs, to stimulate specific areas of the brain that regulate, and are associated with mood.
As the magnetic pulses stimulate the brain, they create neuron activity. Historically, a typical TMS Treatment is administered in regular intervals, in sessions that last anywhere from 30 to 40 minutes.
Newer types of Transcranial Magnetic Stimulation machines are now being used that use shorter protocols and cut the procedure time down to just minutes, like the Theta Burst TMS Machine by MagVenture.
This form of brain stimulus has shown to have a lasting impact on the symptoms of depression and can even provide an improvement in overall mood.
Frontline treatments for depression, such as self-help groups, medications, counseling, and other approaches are often effective for many people.
In some cases, though, patients may suffer negative side effects from medications, or show no sign of improvement over an extended amount of therapy.
Fortunately, Transcranial Magnetic Stimulation has been approved by the Federal Food and Drug Administration (FDA) as a therapy for treatment-resistant depression, or Major Depressive Disorder, when traditional depression treatments have failed to be successful.
There is also growing evidence that TMS Therapy can be effective in treating other mental health issues and even addiction.
TMS Therapy “off-label” uses can include treatment for other disorders like some of the following:
- Post-Traumatic Stress Disorder (PTSD)
- Anxiety Disorders and OCD
- Substance Use Disorders and Addiction
- Chronic pain as a result of injury or disease
- Parkinson’s and Alzheimer’s Disease
- Schizophrenia
- Traumatic Brain Injury (TBI)
- Multiple Sclerosis
TMS Treatment for Depression
October is Depression Awareness Month and a good time to explore causes, symptoms, and effective treatment methods for depression.
While TMS Therapy is not a cure for depression, studies have shown this to be an extremely effective treatment approach when other methods have failed.
More than 50 percent of patients with treatment resistant depression have seen an improvement in their symptoms, while another 37 percent experience total remission of symptoms, according to an observational study published on the Library of Medicine website.
With most treatments, the improvement in symptoms can last up to a year. It’s important to note, though, that depression is caused by a combination of psychological, environmental, and genetic issues, so it’s common for some symptoms to return.
TMS Therapy used in coordination with other treatment methods, such as counseling, regular exercise, balanced nutrition and abstaining from drug and alcohol use can greatly improve a person’s quality of life.
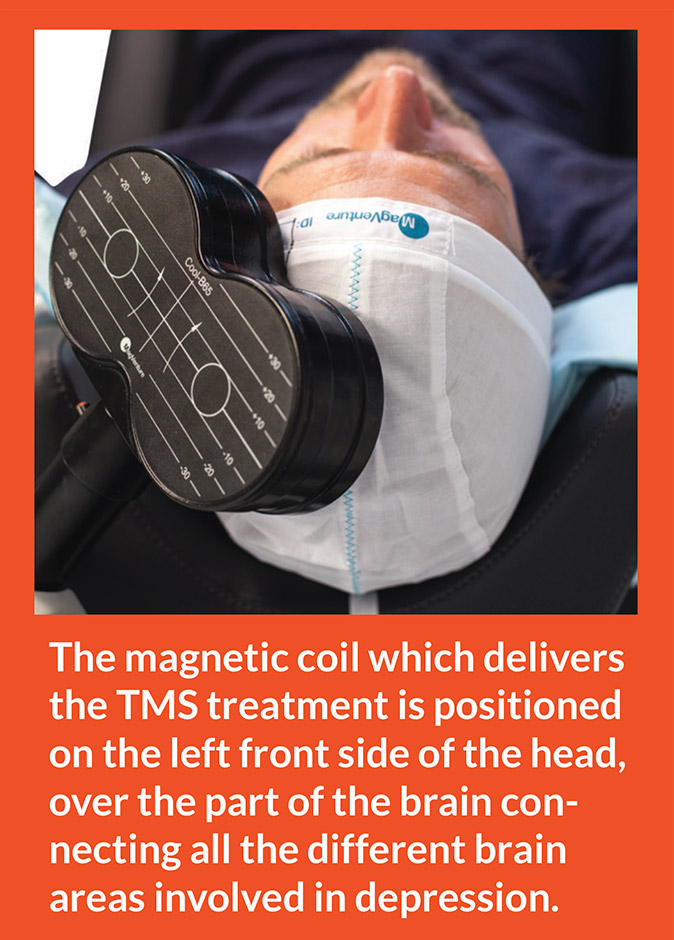
Process of TMS Therapy for Depression
A course of traditional TMS Therapy involves a daily session five times a week, over a period of 4 to 6 weeks. Some patients find it useful to return for supplemental sessions after the initial treatment course.
After being seated in a comfortable chair, a TMS certified clinician provides earplugs and fits a magnetic coil on the patient’s head. During the process, electromagnetic impulses stimulate the brain’s prefrontal cortex located near the forehead.
Earplugs are provided because of the clicking sound produced during the procedure. This is similar to the noise that an MRI makes as it images soft-tissue in the body. Patients may experience a slight tingling sensation on the scalp during and after the process.
Transcranial Magnetic Stimulation Side Effects
Though there are very few side effects with Transcranial Magnetic Stimulation therapy, the ones that do exist are relatively minor and fleeting. About half of the patients experience minor headaches and respond well to over-the-counter pain medications like ibuprofen.
There is no loss of memory or problems with mental focus or acuity after the treatment.
Some patients experience small facial ticks during the procedure, but these tend to dissipate with regular sessions and may even be addressed by the clinicians refitting the coil.
There is an exceedingly low risk for seizure with TMS Therapy, showing less than .01 percent. However, patients with a history of epilepsy or patients with a non-removable metal apparatus in their head do not qualify for TMS.

MagVenture Theta Burst TMS Machine
The FDA approved TMS Therapy as a treatment for major depression in 2008 and for types of migraine headaches in 2011.
The theory and early medical uses of “some form” of Repetitive Transcranial Magnetic Stimulation (rTMS) date back to the late 18th century and it has progressed and been refined ever since.
While there are many types of machines and protocols, the technology has seen quite a few advances in the past decade to reduce the session time from 37 minutes to much lower today.
MagVenture is one such TMS developer. In 2015, they received an FDA clearance for Major Depressive Disorder (MDD) using the 37-minute protocol.
Two years later, in 2017, MagVenture received another FDA clearance using a 19-minute protocol that cut the session time in half.
One year later, they received an FDA clearance for a 3-minute protocol using a Theta Burst Stimulation (TBS).
The Theta Burst TMS technology by MagVenture uses a state of the art machine with very short protocols, so each session takes just a few minutes instead of the usual 37 minutes.
This short treatment session time, combined with the exceptional results for treating major depressive disorder, makes TMS Therapy an ideal solution for patients who have struggled with depression.
TMS Therapy has also shown to be quite effective for people struggling with depression and addiction who fit the profile for this type of treatment.
Related Posts
- Psilocybin Therapy for Depression Treatment and Mental Health
The push to find new and effective treatment approaches for mental health issues like Psilocybin…
- High Functioning Depression Symptoms and Treatment
High Functioning Depression is sometimes called "Functional Depression," but is formally known as “Persistent Depressive…
- Situational Depression Symptoms and Treatment
Life has a way of throwing unexpected curveballs at us that cause stress, anxiety, and…
